| ||||
Mode of Action of Aminoglycoside Antibiotics
Class Notes from Science Prof Online
There are many different classes of antibiotics
each exerting a different type of inhibitory effect that specifically impacts bacteria. Bacterial cells are prokaryotic; primitive cells that differ significantly from humans’ eukaryotic cells.
Aminoglycosides exert their bacteriocidal effect by inhibiting protein synthesis in bacteria and compromising the structure of the bacterial cell wall.
Article Summary: Antibiotics are chemotherapeutic agents used to inhibit or kill bacteria. But how do aminoglycosides destroy these microbes without hurting our cells?
MOA of Aminoglycoside Antibiotics
 | ||||
You have free access to a large collection of materials used in a college-level introductory microbiology course. The Virtual Microbiology Classroom provides a wide range of free educational resources including PowerPoint Lectures, Study Guides, Review Questions and Practice Test Questions.
Page last updated: 5/2014
SPO VIRTUAL CLASSROOMS
 | ||||||
SPO is a FREE science education website. Donations are key in helping us provide this resource with fewer ads.
Please help!
(This donation link uses PayPal on a secure connection.)
Each article in this series covers a specific class of antibiotic and includes the following information:
 | ||||||
HOME MICROBIOLOGY EXPERIMENT FROM SPO
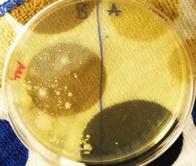
TSY agar with sample from dirty dishes on top (note bacterial colonies that grew), and sample from cleaned dishes on bottom.
Sources & Resources
- Bauman, R. (2014) Microbiology with Diseases by Taxonomy. Pearson Benjamin Cummings.
- Park Talaro, K (2008) Foundations in Microbiology, McGraw Hill.
- Bayarski, Yuri, "Antibiotics and Their Types, Uses and Side Effects."
- Microbiology In the Home: Tips To Sanitize Your House and Keep Your Family Healthy, Household Microbiology article from Science Prof Online.
- Microbial Control Laboratory Exercise Main Page from the Virtual Microbiology Classroom.
- a list of the specific antibiotics that fall in the class (generic and brand names)
- mode of action
- type of infection the antibiotic class to against
- type of bacteria inhibited or killed
- pros and cons of using the class of antibiotics
Main Classes of Antibiotics
- Aminoglycosides
- Cephalosporins (a Beta-lactam)
- Penicillins (a Beta-lactam)
- Quinolones (Fluoroquinolones)
- Sulfonamides (Sulfa Drugs)
Aminoglycoside Antibiotics
Aminoglycoside antibiotics are used to treat serious infections caused by
Some commonly used aminoglycosides include: amikacin (Amikin®); apramycin;
capreomycin; gentamicin (Garamycin®); kanamycin (Kantrex®); neomycin (Mycifradin®); netilmicin (Netromycin®); paromomycin (Humatin®);
streptomycin; tobramycin (TOBI Solution®, TobraDex®, Nebcin®)
Mode of Action
Although aminoglycosides stop bacteria from making proteins, it is uncertain whether this is the action that results in bacterial cell death.
Disruption of Protein Synthesis
Aminoglycosides bind to the bacterial 30S ribosomal subunit. Ribosomes are the protein factories of cells. They are composed of two subunits in bacteria, a 30S and a larger 50S. By binding to the ribosome, aminoglycosides inhibit the translocation of tRNA during translation and leaving the bacterium unable to synthesize proteins necessary for growth.
Although the eukaryotic cells of humans also have ribosomes, these cellular protein factories differ in size and structure from the ribosomes of prokaryotes. That is why aminoglycosides do not interfere with protein synthesis in human cells.
Bacterial Cell Wall Damage
It may not be the inhibition of protein synthesis that produces the bactericidal (bacteria killing) effect. Aminoglycosides also appear to displace cations in the bacterial cell biofilm that are responsible for linking the lipopolysaccharide (LPS) molecules characteristic of Gram-negative bacterial cell walls.
This creates holes in the cell wall that may kill the bacteria before the aminoglycoside even reaches the ribosome. Because our cells do not have cell walls (some of the chemical structural components of the bacterial cell wall are found only bacteria) human cells are not susceptible to these destructive actions.
Type of Infection Aminoglycosides Are Used Against
Aminoglycosides are most often used in empiric therapy (treatment initiated before a firm diagnosis is made) for serious infections including septicemia, complex infections within the abdominal cavity, severe urinary tract infections, and nosocomial (hospital acquired) respiratory infections.
Because of their toxicity, aminoglycosides are only given for only a short period of time. Less toxic antibiotics are substituted once the causative agent of infection is positively identified.
Antimicrobial Spectrum of Aminoglycosides
Gram-negative Aerobic Bacteria: Aminoglycosides exert their antibiotic effect against aerobic (oxygen requiring), gram-negative bacteria, including Pseudomonas, Acinetobacter, and Enterobacter.
Gram-positive Bacteria: Gram-positive bacterial infections can also be treated with aminoglycosides, but are typically not used because of the toxicity. Aminoglycosides have a synergistic effect when combined with beta-lactam antibiotics (penicilins) and have been used to treat streptococcal infections. The ampicillin (a beta-lactam antibiotic) gentamicin combination is referred to as "amp and gent" or "pen and gent" for penicillin and gentamicin.
Mycobacteria: Some species of Mycobacteria, including the causative agent of tuberculosis, are also susceptible to aminoglycosides.
Adverse Effects of Aminoglycosides
Because aminoglycosides are quickly broken down in the stomach, these antibiotics can't be given orally, but instead must be injected.
The adverse effects of aminoglycosides include potential damage to the ears and kidneys. The risk can be reduced by monitoring blood levels of the drug and maintaining the dose at levels that will kill bacteria without causing harmful side effects.
* The information in this article is not meant to be used for self-diagnosis or treatment of illness. If you are sick, seek help from a trained medical professional, not a computer.
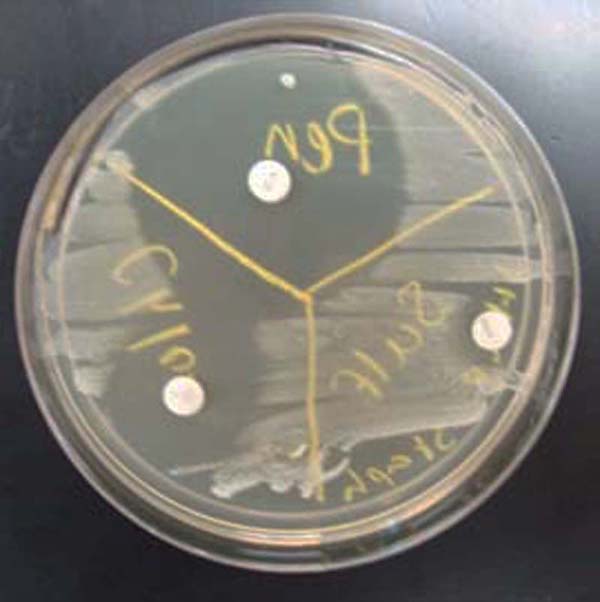
TSY agar inoculated with Staphylococcus. Three antibiotic sensitivity disks appear on this medium: penicillin, sulfa, and ciprofloxacin (clockwise from top). Note the "zone of inhibition" around each antibiotic disk. The larger the zone of bacterial inhibition, the more effective the antibiotic is against the bacteria.
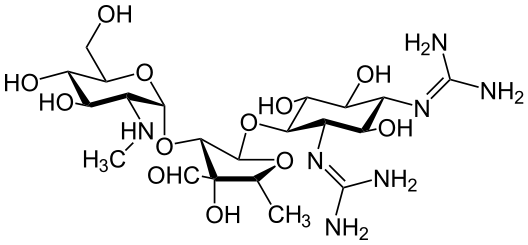
Chemical structure of streptomycin, an aminoglycoside.
 | ||||||